Rosacea
About rosacea
Rosacea is a common but poorly understood long-term skin condition that mainly affects the face.
It can be controlled to some degree with long-term treatment, but sometimes the changes in physical appearance can have a significant psychological impact.
Symptoms of rosacea
Symptoms often begin with episodes of flushing, where the skin turns red for a short period, but other symptoms can develop as the condition progresses, such as:
- burning and stinging sensations
- permanent redness
- spots (papules and pustules)
- small blood vessels in the skin becoming visible
Rosacea is a relapsing condition, which means there are periods when symptoms are particularly bad, but less severe at others.
Read about the symptoms of rosacea
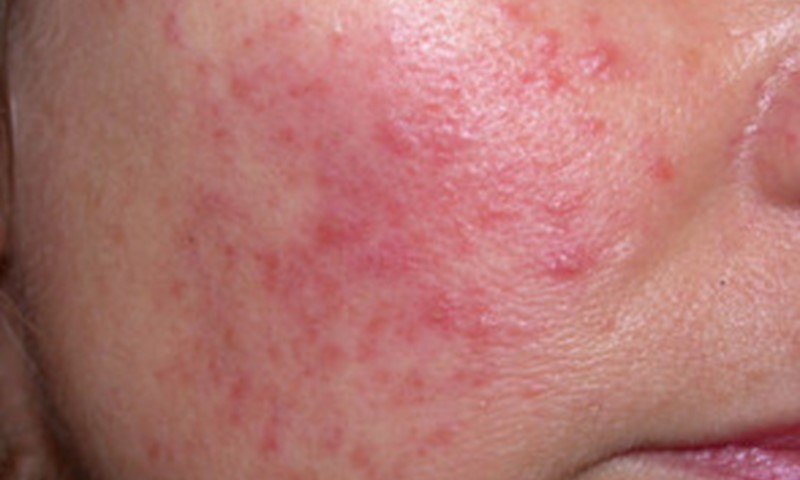
Rosacea symptoms include redness and flushing, as well as stinging and spots.Source: https://dermnetnz.org/
When to see your GP
See your GP if you have persistent symptoms that could be caused by rosacea. Early diagnosis and treatment can help stop the condition getting worse.
There’s no specific test for rosacea, but your GP will often be able to diagnose the condition by:
- examining your skin
- asking about your symptoms
- asking about possible triggers you may have
In some circumstances your GP may arrange further tests to rule out other conditions with similar symptoms, such as lupus or the menopause. For example, these could be a blood test or skin biopsy, where a small scraping of skin is removed and examined.
Causes of rosacea
The exact cause of rosacea is unknown, although a number of possible factors have been suggested, including abnormalities in the blood vessels of the face and a reaction to microscopic mites commonly found on the face.
Although they’re not thought to be direct causes of the condition, several triggers have been identified that may make rosacea worse.
These include:
- exposure to sunlight
- stress
- strenuous exercise
- hot or cold weather
- hot drinks
- alcohol and caffeine
- certain foods, such as spicy foods
Read about causes of rosacea
Treating rosacea
There’s currently no cure for rosacea, but treatment can help control the symptoms.
Long-term treatment is usually necessary, although there may be periods when your symptoms improve and you can stop treatment temporarily.
For most people, treatment involves a combination of self-help measures and medication, such as:
- avoiding known triggers – for example, avoiding drinks containing alcohol or caffeine
- creams and gels – medications applied directly to the skin to reduce spots and redness
- oral medications – tablets or capsules that can help clear up more severe spots, such as oral antibiotics
In some cases procedures such as laser and intense pulsed light (IPL) treatment may be helpful. These involve beams of light being aimed at the visible blood vessels in the skin to shrink them and make them less visible.
Read about more about treating rosacea and self-help measures for rosacea
Living with rosacea
Any long-term (chronic) condition can have an adverse psychological effect, but rosacea can be particularly troublesome as it affects your appearance. This can change how you feel about yourself and how you interact with others.
Many people with rosacea have reported feelings of low self-esteem, embarrassment and frustration.
It’s important to try to come to terms with the fact you have a chronic condition that, although incurable, is controllable.
Persevering with your treatment plan and avoiding your individual triggers are the best ways of controlling your symptoms.
As your physical symptoms improve, you may start to feel better psychologically and emotionally.
If you have rosacea, take comfort in knowing you’re not alone. There are millions of people living with the condition in the UK and across the world.
You can find support and information from organisations like:
- Changing Faces – a charity for people with a visible difference or facial disfigurement, who can be contacted on 0300 012 0275 for counselling and advice
Speak to your GP if you’re feeling depressed as a result of your condition. They may recommend further treatment if necessary.
Ocular rosacea
Rosacea that affects your eyes (ocular rosacea) can lead to a number of eye problems, some of which can be serious.
Symptoms of ocular rosacea can include:
- feeling like there is something in your eyes
- dry eyes
- irritated and bloodshot eyes
- inflammation of the eyelids (blepharitis)
Rosacea can sometimes cause the cornea, the transparent layer at the front of the eyeball, to become inflamed and damaged. This is known as keratitis.
This damage can make the cornea vulnerable to ulceration and infection, which could potentially threaten your sight.
Symptoms of serious problems with your corneas include:
- eye pain
- sensitivity to light (photophobia)
- deterioration in your vision
Contact your GP immediately if you think you may have a problem with your corneas. If this isn’t possible, visit your nearest accident and emergency (A&E) department.
If keratitis isn’t treated promptly by an ophthalmologist, a doctor who specialises in treating eye conditions, there’s a risk of permanent vision loss.
Symptoms of rosacea
Rosacea causes a range of symptoms, although not everyone will experience them all.
Most people with rosacea have periods when their symptoms are particularly troublesome, followed by periods when their symptoms are less so.
The main symptoms of rosacea include:
- flushing
- persistent facial redness
- visible blood vessels
- papules and pustules
- thickened skin
These are discussed in more detail below.
Other symptoms associated with rosacea include:
- sensitive skin – burning, itching, stinging and pain
- dry, rough skin
- raised red patches (plaques) on your skin
- facial swelling (lymphoedema)
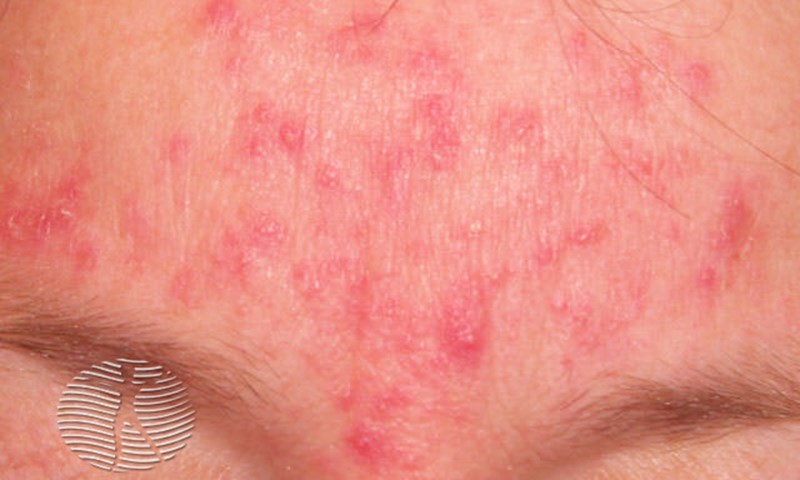
Rosacea can cause different symptoms, including facial redness and flushing.Source: https://dermnetnz.org/
Permanent damage to the face (scarring) almost never occurs in rosacea.
Flushing
Flushing is when your skin turns red for a short period – usually a few minutes. It tends to mainly affect the face, although it can spread to your neck and chest.
In some cases the redness may be accompanied by an unpleasant feeling of heat.
In rosacea flushing is often caused by a certain trigger, such as sun exposure, hot drinks or exercise. See causes of rosacea for more information about possible triggers.
Persistent facial redness
Persistent facial redness (erythema) is like a blush or a patch of sunburn that doesn’t go away, or the sort of blotchy skin often associated with drinking too much alcohol.
This can be upsetting for those with rosacea as people can mistakenly assume they are heavy drinkers.
The redness usually affects the cheeks, nose and chin, but may spread to other areas, such as the forehead, neck and chest.
Visible blood vessels
Over time the blood vessels in the skin may become permanently widened (dilated) and visible. The medical name for visible blood vessels is telangiectasia.
Papules and pustules
If you have rosacea, you may develop round red bumps that rise from your skin (papules) and pus-filled swellings (pustules).
These spots appear on your face and are similar to acne. Rosacea used to be called acne rosacea, but the 2 conditions are quite different.
In rosacea there are no blackheads and the skin is not greasy, but dry and peeling. Rosacea spots also don’t cause scarring.
Thickened skin
In the most serious cases of rosacea the skin can thicken and form excess tissue, usually around the nose. This causes the nose to take on a large, bulbous appearance (rhinophyma).
Rhinophyma is an uncommon, severe symptom of rosacea and takes several years to develop. It almost exclusively affects men.
Causes of rosacea
The exact cause of rosacea is unknown, although a number of potential factors have been suggested.
It’s possible a combination of these factors may be responsible for the condition, although there isn’t enough evidence to say this for certain.
Some of the main factors that have been suggested are outlined below.
Blood vessel abnormalities
Some experts believe abnormalities in the blood vessels of the face may be a major contributing factor for rosacea. This may explain symptoms of flushing, persistent redness and visible blood vessels.
It’s not known what causes these abnormalities. But sun damage may be responsible for degeneration of the elastic tissue of the skin and the dilation of blood vessels.
Skin peptides
Recent research has shown external triggers such as ultraviolet (UV) light, spicy food, alcohol (particularly red wine), exercise, stress, heat and cold can lead to the activation of certain molecules within the skin called peptides.
Increased levels of these peptides may in turn affect the immune system or nerves and blood vessels (neurovascular system) of the skin. Activation of these systems can cause dilation of blood vessels, redness and inflammation.
Microscopic mites
Microscopic mites called demodex folliculorum usually live harmlessly on human skin, but people with rosacea have particularly large numbers, which may play a role in the condition.
It is currently uncertain whether the mite is a cause or an effect of rosacea, although some researchers have suggested the symptoms may be caused by the skin reacting to bacteria in the mites’ faeces.
Helicobacter pylori bacteria
Helicobacter pylori bacteria are bacteria found in the digestive system. It’s been suggested these bacteria may be a possible cause of rosacea, although a link hasn’t been proven.
One theory is the bacteria may stimulate the production of a protein called bradykinin, which is known to cause blood vessels to expand.
Genetics
Rosacea seems to be more common in families, although it’s not clear which genes – if any – are involved or how they’re passed on.
Triggers of rosacea
Although they’re not thought to be direct causes of the condition, many people with rosacea find certain triggers make their symptoms worse.
Different people can have different triggers, but triggers that have been commonly reported include:
- exposure to sunlight
- stress
- hot or cold weather
- strong winds
- strenuous exercise
- alcohol
- hot baths
- spicy foods
- hot drinks
- humidity
- caffeine – found in tea, coffee and cola
- the menopause
- dairy products
- other medical conditions
- certain medicines – such as amiodarone, corticosteroids and high doses of vitamins B6 and B12
Treating rosacea
Although rosacea can’t be cured, treatment can help keep the symptoms under control.
Long-term treatment is usually necessary, although there may be periods where your symptoms improve and you can stop treatment temporarily.
Treatment choices depend on which type of symptom is most troublesome, but usually involves a combination of self-help measures and medication, and are outlined below.
Self-help measures
There are a number of things you can do yourself to help keep the symptoms of rosacea under control, including:
- avoiding things that trigger your symptoms – for example, by using sun cream and covering yourself up if direct sunlight makes your symptoms worse
- taking good care of your skin – for example, by using products suitable for sensitive skin
- using make-up – patches of persistent red skin can be disguised using specially designed camouflage make-up
- keeping your eyelids clean – if rosacea is causing your eyelids to become inflamed (blepharitis)
Treating papules and pustules
If you have round red bumps that rise from your skin (papules) and pus-filled swellings (pustules) caused by rosacea, there are a number of different medications that can be effective.
These can be divided into topical treatments that are applied to the skin, or oral treatments, which are taken by mouth.
Topical treatments
Topical medications are usually prescribed first. These include:
- metronidazole cream or gel
- azelaic acid cream or gel
- ivermectin cream
Ivermectin is a relatively new medicine. There’s some evidence to suggest it may be more effective and perhaps less irritating to the skin than metronidazole, although it’s not currently available on the NHS everywhere and may only be recommended if the other treatments don’t work.
You’ll usually need to apply these topical treatments once or twice a day, taking care not to get them in your eyes or mouth. It may be several weeks before you notice any significant improvement in your symptoms.
Side effects of these treatments can include a burning or stinging sensation, itchiness and dry skin.
Oral antibiotics
If your symptoms are more severe, an oral antibiotic medication may be recommended as these can help reduce inflammation of the skin.
Antibiotics often used to treat rosacea include tetracycline, oxytetracycline, doxycycline and erythromycin.
These medications are usually taken for 4 to 6 weeks, but longer courses may be necessary if the spots are persistent.
For example, a low-dose doxycycline capsule is available if oral antibiotics need to be taken long term.
Common side effects of these medications include:
- feeling and being sick
- diarrhoea
- bloating and indigestion
- tummy (abdominal) pain
- loss of appetite
Some of the medications used can also make your skin sensitive to sunlight and artificial sources of light, such as sun lamps and sunbeds.
As with the topical treatments mentioned above, these medications usually need to be taken once or twice a day and you may not notice a significant improvement in your symptoms for several weeks.
Oral isotretinoin
Isotretinoin is a medicine often used to treat severe acne, but at lower doses it’s also occasionally used to treat rosacea.
As isotretinoin is a strong medication that can cause a range of side effects, it can only be prescribed by a specialist in treating skin conditions (dermatologist) and not your GP.
Common side effects of isotretinoin include:
- dryness and cracking of the skin, lips and nostrils
- inflammation of your eyelids (blepharitis) or eyes (conjunctivitis)
- headaches
- muscle or joint pain
- back pain
- blood in your urine (haematuria)
- mood changes
Isotretinion can also cause birth defects if taken during pregnancy.
Treating facial redness
Treating facial redness and flushing caused by rosacea is generally more difficult than treating papules and pustules caused by the condition.
But as well as the self-help measures mentioned above, there are some medications that can help.
Brimonidine tartrate
Brimonidine tartrate is a relatively new medication for facial redness caused by rosacea. It comes in the form of a gel that’s applied to the face once a day.
The medication works by restricting the widening (dilation) of the blood vessels in your face. Research has shown it can start to have an effect about 30 minutes after it’s first used, and this can last for around 12 hours.
Common side effects of brimonidine tartrate include itchiness and a burning sensation where the gel is applied.
Less common side effects can include:
- a dry mouth
- headaches
- pins and needles
- dry skin
A rebound effect, where flushing becomes worse, has also been reported with this medication.
Oral treatments
Alternatively, there are a number of oral medications that may help improve redness caused by rosacea.
These include:
- clonidine – a medication that relaxes the blood vessels
- beta-blockers – medications that decrease the activity of the heart
- anxiety medications – medications sometimes used to help calm the person and reduce blushing
It’s not clear how effective these medications are at treating redness caused by rosacea, but they may sometimes be prescribed under the supervision of a dermatologist.
Laser and intense pulsed light (IPL) treatment
Redness and visible blood vessels (telangiectasia) can also sometimes be successfully improved with vascular laser or intense pulsed light (IPL) treatment. These treatments may also improve flushing.
A referral to a dermatologist is usually required before having these treatments and they’re not usually available on the NHS, so you may need to pay for them privately. Around 2 to 4 treatments may be needed, so the overall cost may be significant.
Laser and IPL machines produce narrow beams of light that are aimed at the visible blood vessels in the skin. The heat from the lasers damages the dilated veins and causes them to shrink so they’re no longer visible, with minimal scarring or damage to the surrounding area.
Laser treatment can cause pain, but most people don’t need an anaesthetic. Side effects of laser treatment are usually mild and can include:
- bruising
- crusting of the skin
- swelling and redness of the skin
- blisters (in rare cases)
- infection (in very rare cases)
These side effects usually only last a few days and are rarely permanent.
Treating thickened skin
In some people with rosacea the skin of the nose can become thickened. This is known as rhinophyma.
If you have severe rhinophyma, your GP may refer you to a dermatologist or plastic surgeon to discuss ways the appearance of your skin can be improved.
A number of surgical treatments are available to remove any excess tissue and remodel the nose into a more pleasing shape.
This may be done with a laser, a scalpel or specially designed abrasive instruments using a technique called dermabrasion.
Treating eye problems
If rosacea is affecting your eyes (ocular rosacea), you may require further treatment.
For example, you may need to use lubricating eye drops or ointment if you have dry eyes, or oral antibiotics if you have blepharitis.
If initial treatment isn’t effective or you develop any further problems with your eyes, you’ll need to be referred to an eye specialist called an ophthalmologist for further assessment and treatment.
Preventing rosacea
If you have rosacea, there are a number of things you can do to help keep the condition under control.
Avoid triggers
Many people with rosacea notice certain triggers make their symptoms worse. Although it’s not always practical or possible, taking steps to avoid these triggers can help reduce the severity and frequency of your symptoms.
If you’re not sure whether your symptoms have a specific trigger, it may be useful to keep a diary to identify whether your symptoms get worse depending on things like the activities you do and foods or drinks you have.
Advice about how to avoid some common triggers can be found below.
Sunlight
As sunlight is the most commonly reported trigger of rosacea, you should use sun cream whenever possible, even when it’s overcast.
A sun cream with a sun protection factor (SPF) of at least 30 is recommended. A broad-spectrum sun cream that protects against UVA and UVB light should be used.
Using sun creams specifically designed for children may help reduce skin irritation. Covering exposed skin with clothes or a sun hat may also help.
Try to minimise your exposure to the sun during the summer months, particularly in the middle of the day when the sun is at its hottest.
But remember, sun can also be strong in the morning and evening, so take adequate precautions at these times as well.
Stress
Stress is also a commonly reported trigger of rosacea. Successfully managing your stress levels can help control your symptoms.
Ways you can reduce stress include:
- learning relaxation techniques, such as deep breathing exercises, meditation and yoga
- taking regular exercise
As strenuous exercise can sometimes make rosacea symptoms worse, a low-intensity exercise programme, such as walking or swimming, may be better than high-intensity activities, such as running or aerobics.
Read about stress management.
Food and drink
Some of the most commonly reported food- and drink-related triggers are alcohol and spicy foods. You may want to try completely removing these from your diet to see if your rosacea improves.
But there are many other dietary triggers that can also affect some people with rosacea.
It’s a good idea to include information about how your diet affects your rosacea symptoms in your rosacea diary.
Cold weather
Covering your face and nose with a scarf can help protect your skin from cold temperatures and wind.
If you need to spend considerable time outside during cold weather, protect your face with a balaclava.
Skincare techniques
The advice below about skincare techniques may also help control your rosacea symptoms.
- Clean your skin every morning and evening using a gentle, non-abrasive cleanser. Use soap-free cleansers with non-alkaline or neutral pH. Avoid scented soaps and alcohol-based skin cleansers
- Rinse your face with lukewarm water and allow skin to dry thoroughly before you apply medication or make-up
- Look for products suitable for sensitive skin. These are usually described as mild, hypoallergenic, fragrance-free and non-comedogenic (will not block pores)
- Use a moisturiser to soothe skin if it feels sore
- Avoid oil-based or waterproof cosmetics requiring solvents for removal. Use water-based make-up and skin products instead
- Avoid astringents, toners and other facial or hair products that contain ingredients that might irritate your skin, such as fragrances, alcohol, menthol, witch hazel, eucalyptus oil, camphor, clove oil, peppermint, sodium lauryl sulphate and lanolin
- You may want to avoid using anything on your skin that you aren’t sure of. You can then gradually reintroduce products once your symptoms have been treated and cleared to see if you can use them again without any problems
- Men may find that using an electric razor, rather than a blade, helps reduce skin irritation
- Some people find regular gentle facial massage reduces swelling (lymphoedema)
- Don’t use steroid cream unless you’re specifically instructed to by your GP, as it may make your symptoms worse
Skin camouflage
It may be possible to disguise patches of persistent red skin using specially designed camouflage make-up.
The charity Changing Faces offers a skin camouflage service, available nationally and free of charge, to help with the use of these creams.
Your GP or dermatologist can refer you to the skin camouflage service and prescribe skin camouflage make-up.
Eyelid hygiene
If your eyelids are inflamed as a result of rosacea (blepharitis), cleaning your eyelids every day with warm water and a small amount of cleaning solution can help ease your symptoms.
Avoiding eye make-up can also help reduce your symptoms, but if you do choose to wear eye make-up, make sure it is a type that washes off easily so you can still clean your eyelids.
Last updated:
22 February 2023
